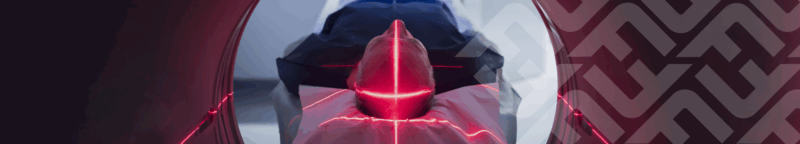
Introduction
From spinal cord stimulation to transcranial magnetic stimulation (TMS) and emerging focused ultrasound systems, neuromodulation has become one of the most dynamic frontiers in medical technology. These devices hold the promise of modulating neural activity to treat conditions as diverse as chronic pain, movement disorders, depression and epilepsy. But transforming an innovative concept into an approved, market-ready therapy requires navigating a complex web of scientific, clinical and regulatory challenges.
At Franklyn Health, our team has supported device manufacturers at every stage, from early feasibility to pivotal trials, and have seen that the most successful teams focus on five key considerations from the outset.
Understand Your Regulatory Classification Early

A neuromodulation device’s regulatory pathway determines everything that follows: study design, data requirements, approval timelines and cost. In the US, Europe and UK, classification depends on intended use, mechanism of action and risk level. Risk factors such as patient population and clinician-led or patient-led use can bump up the overall risk profile.
- USA: Most neuromodulation devices that have a comparable, legally marketed predicate are reviewed through the 510(k) pathway as Class II devices with special controls. Novel systems without a predicate may instead follow the De Novo classification route to establish a new Class II category. If a device introduces higher risk (such as implantable or closed-loop stimulation systems that adjust parameters automatically), the FDA may classify it as Class III, requiring a Premarket Approval (PMA) submission supported by an Investigational Device Exemption (IDE) pivotal study.1, 2.
- Europe and UK: Under the EU MDR and UK MDR, neuromodulation systems that deliver energy to the central nervous system are generally Class IIb (or Class III for deeper or higher-risk stimulation). Clinical investigation is almost always required, as equivalence arguments are difficult under MDR’s stricter rules3, 4.
Early engagement with regulators, either through FDA pre-subs or EU Notified Body consultations, can de-risk your device’s development dramatically. As a rule of thumb, treat classification not as a box-ticking step but as the foundation of your entire evidence strategy.
Build a Clinical Evidence Plan That Proves Both Safety and Precision

Neuromodulation devices are unique in that how precisely and safely they deliver energy can be as important as whether they work. Regulators now expect quantitative proof of targeting accuracy and closed-loop control, not just clinical outcomes.
Well-constructed feasibility data (typically 30 – 60 subjects) is invaluable for refining stimulation parameters, verifying usability and shaping the pivotal trial design. A clear, phased evidence roadmap helps ensure every dataset contributes toward regulatory approval rather than duplicating effort later.
In the US, pivotal studies are typically randomised, sham-controlled and double-blind, powered to show a meaningful improvement on validated scales (for example, MADRS or HAM-D in psychiatric studies, or pain-intensity reduction for chronic-pain indications)5, 6.
The FDA and EU/UK MDR both emphasise:
- Navigation accuracy – Demonstrate millimetre-level targeting repeatability against a neuronavigation reference.
- Closed-loop safety – Pre-specify control objectives, latency limits and fail-safe logic.
- Human-factors validation – Especially critical for home-use devices; summative studies in lay users are essential.7
- Cybersecurity and telemetry integrity – Regulators will expect secure data transmission, safe loss-of-connectivity behaviour, and validated over-the-air update processes.8
Treat Software and Algorithms as Regulated Medical Components

In modern neuromodulation systems, the app and firmware are generally not considered accessories per FDA or EU MDR definitions, but as integral components of the medical device. The key test is whether software drives, controls, analyses or influences the device’s function, then it’s considered part of the therapy and is regulated depending on how the software and hardware are integrated:
- Integrated Software (app + stimulator = one system): one submission, but app lifecycle, validation and cybersecurity requirements apply
- Standalone app that analyses/prescribes stimulation: separate SaMD and the class may equal or exceed the device class
- Accessory app that monitors or records, but has no control: it may be considered an accessory level per MDR (though still needs CE marking)
Key standards apply across all regions:
- IEC 62304 for software lifecycle management
- ISO 14971 for linking software hazards to system risk
- IEC 62366-1 for usability (particularly with lay users)
- IEC/TR 60601-4-5 and FDA’s 2023 cybersecurity guidance for connected systems9,10
If the control algorithm uses adaptive or AI-based logic, expect additional requirements for change management, performance drift monitoring and bias evaluation across user demographics11. Under the MDR’s Rule 11, even a companion app that guides placement or monitors treatment may be classified as a medical device in its own right3.
Establishing robust design-control documentation early is key. Think architecture diagrams, unit and integration testing and validation protocols. Getting this right from the beginning can save months of rework when the technical file is assembled.
Balance Innovation with Real-World Usability
The promise of home-use neuromodulation depends on one deceptively simple question: can ordinary people use it safely and correctly every day?
Human-factors engineering (per IEC 62366-1) is no longer optional. Regulators expect evidence from summative usability studies that simulate real-world conditions: donning headgear, pairing apps, starting sessions, responding to alarms and pausing treatment if something goes wrong7.
Equally, clinical success depends on adherence and engagement. Devices that integrate intuitive interfaces, remote monitoring and clear feedback loops see markedly higher compliance rates12. Connected systems that transmit telemetry to clinicians enable early intervention when protocols drift, benefiting both safety and data completeness.
From a commercial standpoint, usability is also your moat. A system that’s easier to train, maintain and integrate into clinical workflows can shorten adoption curves and lower the total cost of ownership for hospitals and practices.
Plan for Post-Market Evidence and Lifecycle Management
Market authorisation is not the finish line; it’s the start of a continuous-evidence cycle. Under the EU/UK MDR frameworks, manufacturers must maintain a Post-Market Clinical Follow-Up (PMCF) plan and update clinical evaluations with real-world data3,13. Similarly, the FDA may require post-approval studies or special-control surveillance for De Novo or PMA devices1,14.
For neuromodulation products, particularly those involving adaptive algorithms or home use, ongoing data collection demonstrates sustained performance and informs updates to firmware, algorithms and labelling. Sponsors should define, early on:
- What data will be collected post-market (e.g. safety events, adherence, QoL outcomes).
- How software updates will be validated and documented under a controlled QMS.
- When to trigger re-submission to Notified Bodies/regulators for significant algorithmic or functional changes.
An ISO 13485-compliant quality management system is indispensable here. It ties together design controls, CAPA, software updates, and vigilance reporting, providing the audit trail regulators expect15.
The Cost of Getting It Right (and the Cost of Getting It Wrong)
A well-planned neuromodulation development programme typically spans three years and £7–10 million across R&D, feasibility, pivotal studies and regulatory submissions. As much as half that budget can go towards clinical studies, with the remainder divided among software validation, non-clinical testing and manufacturing scale-up.
The temptation to cut corners almost always backfires, for example delaying usability testing or under-powering a feasibility study. A device that fails human-factors testing or produces ambiguous clinical data can lose a full year to redesigns and repeat studies. The cost of missing data can be existential.
Early strategic planning, combined with experienced clinical partners, protects both time and investment.
Why Experience Matters
At Franklyn Health, we work exclusively with small and midsize medtech innovators. Our teams have led global device studies under both FDA IDE and EU MDR frameworks, helping clients navigate feasibility, pivotal and post-market phases with agility and senior-level oversight throughout.
We believe medtech innovators deserve a partner who values responsiveness, transparency and true scientific engagement; not a one-size-fits-all CRO approach. Whether you’re designing a feasibility protocol, preparing a De Novo submission or aligning your MDR clinical strategy, our mission is to make regulatory-grade evidence achievable for growing device companies.
Key Takeaway
Bringing a neuromodulation device to market demands both innovation, careful planning and discipline. By defining your regulatory pathway early, building a robust and targeted evidence plan, treating software as part of the device, prioritising usability and planning for post-market evolution, manufacturers can de-risk their device’s development and accelerate patient access to transformative therapies.
References
- U.S. Food and Drug Administration. Investigational Device Exemptions (IDE) Regulations – 21 CFR Part 812.
- U.S. Food and Drug Administration. De Novo Classification Process (Final Guidance, 2023).
- European Parliament and Council. Regulation (EU) 2017/745 on Medical Devices (MDR).
- Medicines and Healthcare products Regulatory Agency (MHRA). UK MDR 2002 (as amended).
- George, M.S. & Aston-Jones, G. (2010). Noninvasive techniques for probing neurocircuitry and treating illness: vagus nerve stimulation (VNS), transcranial magnetic stimulation (TMS), and transcranial direct current stimulation (tDCS). Neuropsychopharmacology Reviews, 35(1), 301–316.
- FDA Center for Devices and Radiological Health. Premarket Approval (PMA) Clinical Investigations Guidance, 2021.
- IEC 62366-1:2015. Application of Usability Engineering to Medical Devices.
- FDA. Cybersecurity in Medical Devices: Quality System Considerations and Content of Premarket Submissions (Final Guidance, 2023).
- IEC 62304:2006 + A1:2015. Medical Device Software – Software Lifecycle Processes.
- ISO 14971:2019. Application of Risk Management to Medical Devices.
- FDA. Artificial Intelligence and Machine Learning Software as a Medical Device (AI/ML SaMD) Action Plan, 2021.
- Peterchev, A.V. et al. (2012). Transcranial Magnetic Stimulation: Methods and Clinical Applications. Clinical Neurophysiology, 123(11): 2220–2232.
- MDCG 2020-7. Post-Market Clinical Follow-Up (PMCF) Plan Template.
- FDA. Postmarket Surveillance Under Section 522 of the Federal Food, Drug, and Cosmetic Act.
- ISO 13485:2016. Medical Devices – Quality Management Systems.